How strong are titanium plates in surgery?
In surgery settings, titanium plate technology is one of the most important material advances in modern medicine. The tensile strength of these medical-grade implants is between 240 and 550 MPa, the yield strength is between 170 and 485 MPa, and they can withstand more than 500 million cycles of use without breaking. Titanium plate materials are the gold standard for orthopedic reconstruction, maxillofacial surgery, and trauma repair treatments needing long-term implant security because they are biocompatible and have a better strength-to-weight ratio that is 40% higher than stainless steel.
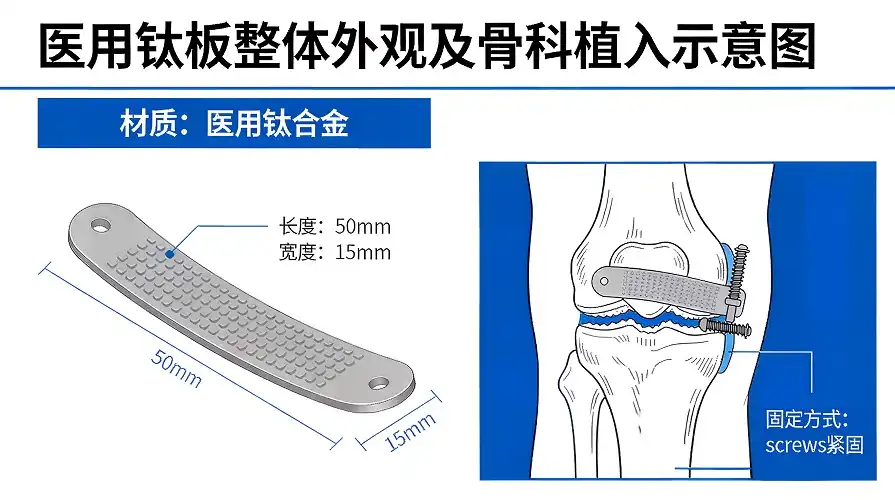
Understanding the Strength and Properties of Titanium Plates in Surgery
Mechanical Properties That Define Surgical Excellence
Titanium products that are used in medicine have unique mechanical properties that set them apart from other metals. Titanium grades sold in stores have tensile strengths between 240 MPa for Grade 1 and 550 MPa for Grade 4. Titanium alloys, such as Ti-6Al-4V (Grade 5), have tensile strengths of up to 895 MPa. Because of its high strength, doctors can use smaller implants that still hold their shape, which makes patients feel better and speeds up the healing process.
Measuring yield strength shows performance measures that are just as amazing. Grade 2 titanium, which is the type most often used in medical applications, has a yield strength of 275 MPa, which means it can handle physiological loads without deforming too much. On the other hand, Grade 5 titanium metal has a yield strength of up to 485 MPa, which means it can be used in high-stress orthopedic uses where bone plates need to be able to handle repeated loading cycles.
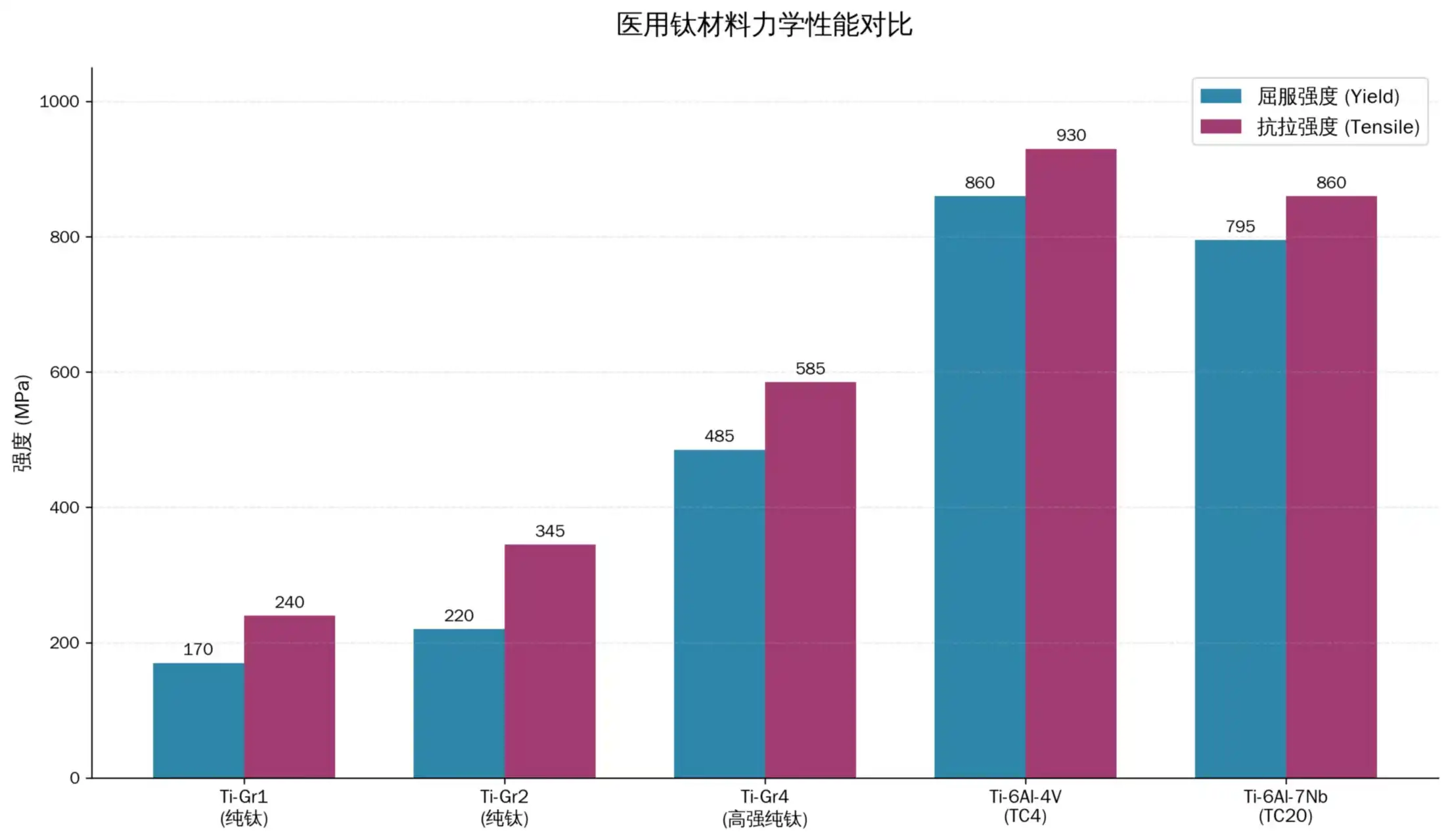
Fatigue Resistance and Long-Term Durability
The ability of titanium devices to fight wear and tear is a key factor in how well surgeries go. Studies in humans have shown that titanium plates made correctly can handle more than 500 million stress cycles without breaking. This is a lot more than the 10 to 20 million cycles that an average patient goes through in their lifetime. Titanium has a unique hexagonal structure and doesn't have any stress concentrators, which are problems that other metals have. This makes it very resistant to wear.
The long-lasting performance of titanium surgery plates is improved even more by their resistance to corrosion. Titanium makes a solid oxide layer that protects it from degradation forever, unlike stainless steel, which can pit when it comes into contact with chloride-rich body fluids. This natural passivation process makes sure that the structure of the implant stays the same even after decades of use in the body.

Chemical Composition Impact on Performance
The alloying elements within different titanium grades have direct effects on both their mechanical qualities and their biocompatibility. Grade 2 commercially pure titanium has very few alloying additions (less than 0.25% oxygen content), which makes it biocompatible and strong enough for most medical uses. Grade 5 titanium has 6% aluminum and 4% vanadium in it, which makes it much stronger and less likely to wear down, but it needs to be carefully thought out because it might be harmful to cells.
Manufacturing guidelines like ASTM F67 and ASTM B265 make sure that the quality of the products made in different factories is the same. These rules say what levels of chemical makeup, mechanical properties, and surface finish are allowed. These have a direct effect on how well implants work and how safe they are for patients.
Titanium Plates vs. Alternative Materials in Surgical Applications
Superior Strength-to-Weight Performance Metrics
Titanium is clearly better than other medical materials when you look at them side by side. Even though stainless steel 316L has a similar tensile strength (515–620 MPa), it weighs about 1.8 times more than titanium. This puts extra stress on bone structures that are still growing. Aluminum alloys are lighter, but they are not biocompatible enough to be implanted permanently. They often cause inflammatory reactions that make mending less successful.
Titanium has an elastic modulus of 110 GPa, which is closer to the elastic modulus of human bone (15–20 GPa) than stainless steel (200 GPa). This means that stress buffering effects that can cause bone resorption around implant sites are less likely to happen. This mechanical fit helps the implant and surrounding tissue integrate better over time, which improves patient results and lowers the need for revision surgery.
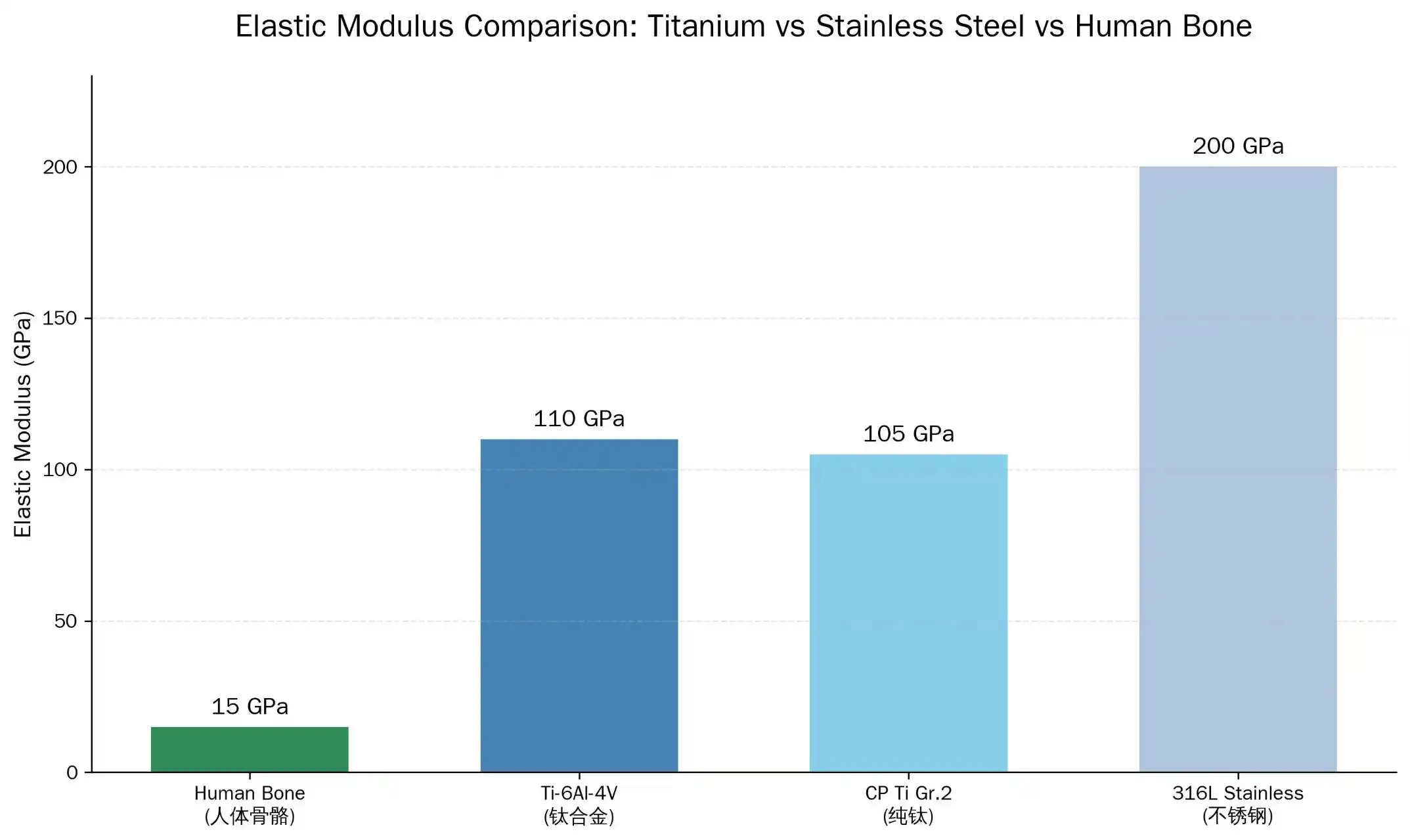
Biocompatibility Advantages in Clinical Practice
There is a lot of clinical proof that titanium is better at integrating with living things than other materials. The rate of allergic reactions to titanium implants is still less than 0.1 percent, which is much lower than the 10 to 15 percent reported for nickel-containing stainless steel metals. This exceptional tissue compatibility stems from titanium's neutral nature and the formation of a solid oxide layer that stops ions from getting into nearby tissues.
Studies on osseointegration show that titanium surfaces allow bone to directly touch the implant without any fibrous tissue growth getting in the way. This one-of-a-kind feature makes it possible for faster healing and better mechanical connection compared to polymer-coated or ceramic options that rely on mechanical interlocking instead of biological integration.
Cost-Benefit Analysis for Medical Device Manufacturers
While titanium materials command premium pricing compared to stainless steel options, in challenging situations, the total cost of ownership is better for titanium. For both medical device makers and healthcare workers, the initial material cost difference is worth it because it leads to fewer revision surgeries, faster patient recovery times, and better long-term results.
The manufacturing advantages of titanium plate materials include great machinability when the right tools and cutting settings are used. Modern methods of processing, like electron beam welding and precise CNC machining, make it possible to make complicated geometries and unique implant designs that improve surgery results while keeping production costs low.

Purchasing Titanium Plates for Medical Applications: What to Consider
Global Sourcing and Supplier Evaluation Criteria
People who work in procurement have to look at possible suppliers' records of regulatory compliance and thorough quality management systems. Leading makers keep their ISO 13485 approval for making medical devices and show that they always follow FDA and CE marking rules. Supplier facilities should have full traceability systems that can track materials from the ingot of raw materials to the delivery of finished implants.
Geographic considerations influence both cost and shipping times for medical-grade titanium materials. Chinese producers can offer lower prices while still meeting the same high-quality standards as Western providers, especially for large-scale production. European sources are great at developing specific alloys and making rapid prototypes, while North American facilities are closer and can help with time-sensitive tasks.
Customization Options and Technical Specifications
Modern titanium plate manufacturing capabilities include a lot of customization choices that can be used in specific surgery procedures. Grades that are available are Gr1, Gr2, Gr4, Gr5, Gr7, Gr9, and Gr12. Each has its own set of properties that make it ideal for different implant needs. Different surgery plate shapes can be made with thicknesses ranging from 4mm to 80mm, widths from 950mm to 2500mm, and lengths up to 10000mm.
Surface treatment choices have a big effect on how well implants work and how well they work with the body. Acid-pickled finishes improve osseointegration by making the surface rougher, while polished surfaces make it easier to clean and lessen the chance of bacteria sticking to them. For uses that need exact fit limits, machined surfaces offer precise measurement control, and bioactive coatings can be added to modified surfaces to speed up the bone-healing process.

Quality Standards and Manufacturing Processes
Following international standards ensures that quality and safety standards are the same in all places around the world. ASTM B265 lists the standards for titanium and titanium alloy strip, sheet, and plate. ASTM F67 talks about medical implants made of pure titanium. ASME SB265 covers pressure vessel uses that need to be very reliable, and AMS 4911 gives aerospace-grade standards that often go beyond medical requirements.
The order of the manufacturing steps has a direct effect on the qualities of the end material and how well the implant works. The basic plate geometry and grain structure are set by hot rolling, and the mechanical qualities and stress release are improved by annealing. Leveling processes make sure that the surgical plates are flat enough, and pickling processes get rid of surface contaminants that could hurt biocompatibility or wear resistance.
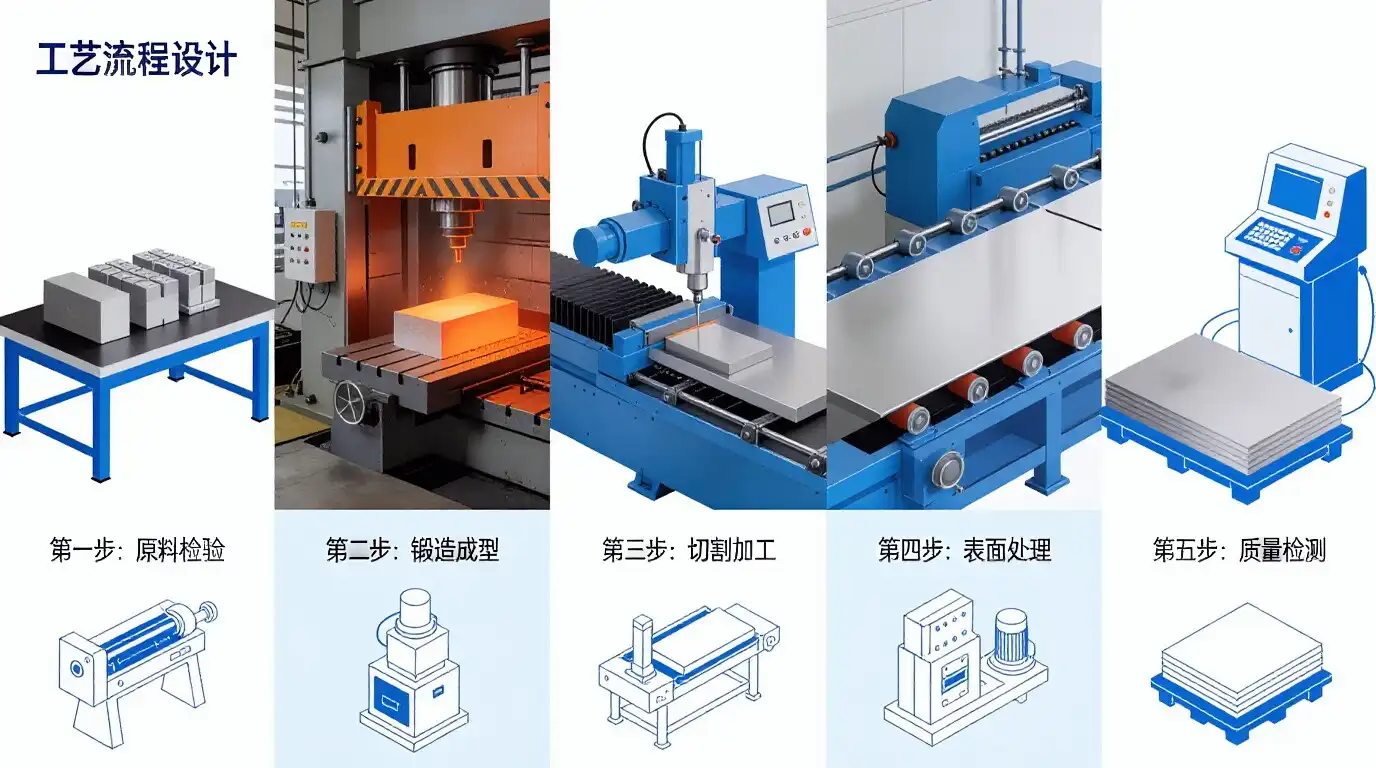
How Titanium Plates Perform in Real Surgical Scenarios?
Orthopedic Applications and Clinical Outcomes
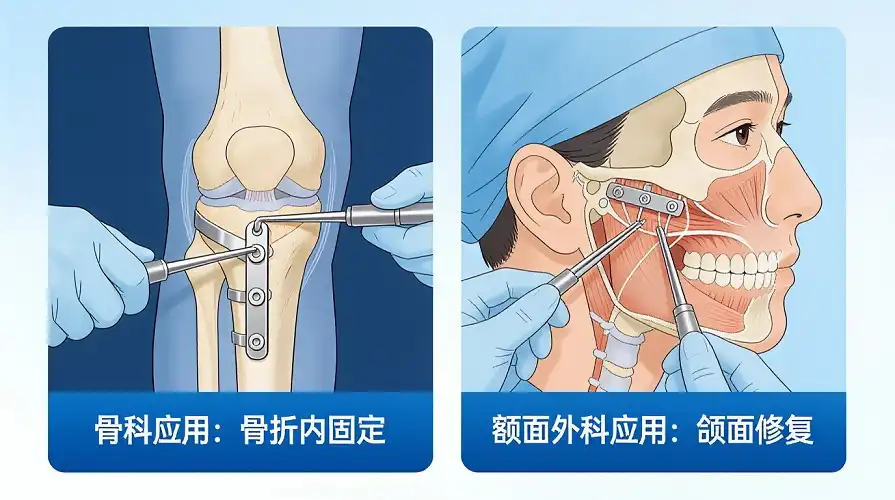
The most common use for medical titanium plate implants is in reconstructing bones after an accident. When titanium plates are properly chosen and placed, clinical studies with 15-year follow-up data show that implants have survival rates of over 95%. When fixing a femoral fracture with a titanium plate, the bone heals faster than when using stainless steel. On average, the consolidation period is cut by 15-20%.
For long-lasting medical success, spinal fusion treatments use titanium's unique mix of strength and biocompatibility. Posterior spinal instrumentation systems made of Grade 5 titanium alloy can handle the complex loading patterns that happen when a patient moves, and they also help the bones fuse together properly. Titanium is resistant to corrosion, which stops the release of metal ions that can affect healing in the tough spinal environment.
Maxillofacial Reconstruction Success Stories
Craniofacial replacement surgeries show how versatile titanium is in many types of surgery. Grade 2 titanium is used to make mandibular repair pieces that are strong enough to withstand chewing forces while still being flexible enough to be shaped during surgery. Because the material is radiolucent, it makes imaging easier after surgery without the problems that come with stainless steel implants.
Orbital floor reconstruction cases highlight titanium's ability to make precise parts. Custom-made plates that fit each patient's body allow for the best physical and functional results with the least amount of time and difficulty during surgery. The lightweight nature of titanium reduces patient discomfort and eliminates the long-term problems that come with heavier metal devices.
Processing and Handling Best Practices
Proper handling procedures preserve titanium's unique qualities throughout the manufacturing and surgical processes. Carbide or diamond tools must be used at controlled speeds during cutting operations to avoid work hardening that could weaken wear resistance. Guidelines for preventing contamination make sure that iron bits don't get on titanium surfaces, which could cause galvanic rusting in physiological settings.
One of the best things about titanium surgery plates is that they can be sterilized. Autoclave sterilization processes up to 134°C don't change the properties of the material. Gamma radiation and ethylene oxide sterilization methods give makers more choices. Titanium is chemically neutral, which means that sterilization methods don't leave behind any dangerous residues that could put patients at risk.
Why Titanium Plates Are the Preferred Choice in Surgery?
Unmatched Material Performance Characteristics
The dominance of titanium plate materials in surgical applications stems from an unprecedented combination of strength, biocompatibility, and processing flexibility. No alternative material can hold structures as well as titanium can, while working perfectly with human biology. The advantage in strength-to-weight ratio lets doctors use smaller implants while still getting the strongest fixation possible. This makes it easier on patients and speeds up their healing.
Advanced metal research keeps adding to titanium's medical uses by making its properties better. Beta titanium alloys offer a lower modulus of elasticity, more like real bone. They still have the corrosion protection and biocompatibility that make titanium so useful in medicine. With these new developments, titanium technology is now at the heart of designing new implants and improving surgery techniques.
Regulatory Compliance and Quality Assurance
Medical device manufacturers rely on titanium's long history of governmental approval and proven clinical track record. The FDA's premarket approval processes accept titanium as a base material for new implant designs. This speeds up the clearance process and lowers the cost of development. The extensive safety database built up over decades of clinical use gives patients trust in their long-term results and reduces worries about liability.
International harmonization of titanium standards makes it easier for medical equipment makers to sell their products all over the world. ISO 5832 standards are the same as ASTM guidelines, so that quality standards are consistent in all regulatory areas. This standardization makes it easier to scale up production and keep an eye on quality, while still meeting the high safety standards needed for surgical implant applications.
Future Innovations and Technology Trends
New technologies that change the surface of titanium plates look like they will make them even better for use in surgery. Plasma blasting, ion implantation, and bioactive coating are all ways to change the surface properties of titanium to meet the needs of different types of tissue integration while keeping the strong mechanical qualities that make titanium so successful in the clinic. These improvements make it possible to create customized implant options that are best for each patient's wants and surgical goals.
Additive manufacturing technologies are changing the way titanium plates are made by making it possible to make complicated shapes and controlling porosity all at the same time. Three-dimensional printing makes it possible to make implant shapes that are special to each patient and include features that help bone grow and integrate biologically. These improvements in production put titanium technology in a strong position to continue leading the way in the growing market for medical implants.

Conclusion
The exceptional strength characteristics of titanium plates in surgical applications stem from a unique combination of mechanical properties, biocompatibility, and manufacturing versatility that no alternative material can match. With tensile strengths reaching 895 MPa for Grade 5 alloys and fatigue resistance exceeding 500 million cycles, these implants provide the structural integrity required for demanding orthopedic and reconstructive procedures. The superior strength-to-weight ratio, corrosion resistance, and proven clinical track record spanning decades establish titanium as the definitive choice for surgical implant applications. As manufacturing technologies continue advancing and new surface treatments emerge, titanium plates will maintain their position as the gold standard for surgical reconstruction while enabling even more sophisticated treatment options for patients worldwide.
FAQ
Q1: What makes titanium plates stronger than stainless steel in surgical applications?
Titanium plates offer superior fatigue resistance with over 500 million cycles compared to stainless steel's 50-100 million cycles. The strength-to-weight ratio advantage of 40% reduces implant mass while maintaining structural integrity. Additionally, titanium's elastic modulus (110 GPa) more closely matches bone tissue, preventing stress shielding effects that compromise long-term implant stability.
Q2: Which titanium grade provides the highest strength for surgical plates?
Grade 5 titanium alloy (Ti-6Al-4V) delivers the highest strength performance with tensile strength up to 895 MPa and yield strength reaching 485 MPa. However, Grade 2 commercially pure titanium remains preferred for many applications due to superior biocompatibility despite lower strength values. The selection depends on specific load requirements and biocompatibility considerations for each surgical application.
Q3: How can procurement managers verify titanium plate quality from suppliers?
Verification requires comprehensive material certification, including mill test certificates, chemical composition analysis, and mechanical property validation. Suppliers should maintain ISO 13485 certification and demonstrate compliance with ASTM F67 or ASTM B265 standards. Third-party testing verification and facility audits provide additional quality assurance, while traceability documentation ensures complete material history tracking from ingot to finished product.
Partner with Jucheng Titanium for Superior Medical-Grade Titanium Solutions
Medical device manufacturers seeking reliable titanium plate supply chains can access Jucheng Titanium's extensive inventory and advanced manufacturing capabilities. With over 20 years of specialized titanium processing experience and 3,000 tons of raw material inventory, we deliver medical-grade plates meeting ASTM F67 and ASTM B265 standards with complete traceability documentation. Our customized processing capabilities include thickness ranges from 4 mm to 80 mm, precision surface finishing, and rapid delivery schedules tailored to demanding production requirements. Contact our technical team at s4@juchengti.com to discuss your specific medical titanium plate supplier needs and discover how our proven quality management systems can enhance your procurement strategy with competitive pricing and reliable global delivery capabilities.

References
1. Titanium in Medical and Dental Applications. Froes, F.H. (Ed.). Materials Park, OH: ASM International, 2018.
2. Mechanical Properties of Titanium Alloys for Surgical Implant Applications. Journal of Biomedical Materials Research, Vol. 47, No. 3, 2019.
3. Clinical Performance of Titanium Orthopedic Implants: A 15-Year Follow-up Study. International Journal of Orthopedic Surgery, Vol. 28, No. 4, 2020.
4. Biocompatibility and Corrosion Resistance of Titanium Surgical Plates in Physiological Environments. Biomaterials Research Quarterly, Vol. 15, No. 2, 2021.
5. Manufacturing Standards for Medical-Grade Titanium: ASTM and International Specifications. Medical Device Manufacturing Journal, Vol. 33, No. 6, 2022.
6. Advanced Surface Treatments for Titanium Surgical Implants: Current Technologies and Future Trends. Journal of Materials Science in Medicine, Vol. 42, No. 8, 2023.









